Search
- Page Path
- HOME > Search
Case Report
- Bilateral Xanthogranulomatous Pyelonephritis With Extensive Abscess Associated With Neurogenic Bladder: A Case Report
- Sin Woo Lee, Hee Seung Choi
- Urogenit Tract Infect 2026;21(1):40-43. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550026013
-
 Abstract
Abstract
 PDF
PDF PubReader
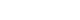
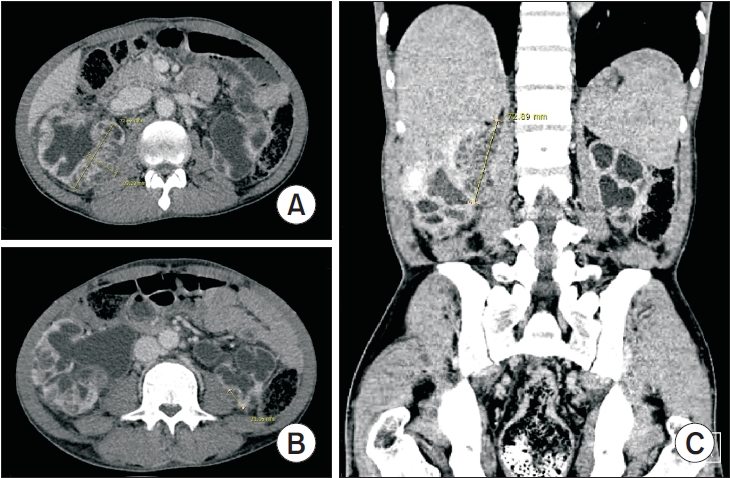
PubReader - Xanthogranulomatous pyelonephritis (XGP) is a rare and severe form of chronic pyelonephritis. We report a case of bilateral XGP complicated by extensive abscess formation. A 47-year-old man presented with fatigue and generalized weakness. Laboratory evaluation revealed leukocytosis and elevated serum creatinine levels. Urinalysis demonstrated pyuria and bacteriuria. Computed tomography (CT) revealed bilaterally enlarged kidneys with multifocal renal parenchymal and perirenal abscesses. The CT scan also demonstrated severe bilateral hydronephroureter and diffuse bladder wall thickening, with a radiologic impression of severe pyelonephritis with abscess formation and neurogenic bladder. The patient was admitted and treated with intravenous antibiotics and percutaneous nephrostomy tube placement. However, no clinical improvement was observed with conservative management. The patient subsequently underwent right open radical nephrectomy. Histopathological examination confirmed the diagnosis of XGP with extensive abscess formation. The patient experienced no further complications or recurrence after surgery. This case suggests that chronic untreated neurogenic bladder may contribute to the development of severe chronic pyelonephritis such as XGP.
- 207 View
- 7 Download

Original Articles
- Mortality and Risk Factors for Emphysematous Pyelonephritis in Korea: A Multicenter Retrospective Cohort Study
- Seung-Kwon Choi, Jeong Woo Lee, Seung Il Jung, Eu Chang Hwang, Joongwon Choi, Woong Bin Kim, Jung Sik Huh, Jin Bong Choi, Yeonjoo Kim, Jae Min Chung, Ju-Hyun Shin, Jae Hung Jung, Hong Chung, Sangrak Bae, Tae-Hyoung Kim
- Urogenit Tract Infect 2025;20(1):34-41. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2550006003
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose
Emphysematous pyelonephritis (EPN) is a life-threatening disease requiring immediate treatment. This multicenter retrospective cohort study aimed to analyze the mortality rate and risk factors associated with EPN. Materials and Methods: Between January 2011 and February 2021, 217 patients diagnosed with EPN via computed tomography who visited 14 teaching hospitals were retrospectively analyzed. Clinical data, including age, sex, comorbidities, Huang and Tseng classification, hydronephrosis, acute kidney injury, blood and urine tests, surgical interventions, percutaneous drainage, and conservative treatments, were compared between the survival and death groups. Risk factors for mortality due to EPN were analyzed using univariate and multivariate methods.
Results
The mean age of survivors and deceased patients was 67.8 and 69.0 years, respectively (p=0.136). The sex distribution (male/female) was 48/146 and 8/15, respectively (p=0.298). Of the 217 patients, 23 died, resulting in a mortality rate of 10.6%. In univariate analysis, the Huang and Tseng classification (p=0.004), platelet count (p=0.005), and acute kidney injury (p=0.007) were significantly associated with mortality from EPN. In multivariate analysis, only the Huang and Tseng classification (p=0.029) was identified as a risk factor. Mortality rates according to the Huang and Tseng classification were as follows: class I (5.88%), class II (7.50%), class IIIa (14.28%), class IIIb (25.00%), and class IV (23.07%).
Conclusions
EPN is associated with a high mortality rate. Among various clinical factors, the Huang and Tseng classification was the most significant indicator for predicting mortality. -
Citations
Citations to this article as recorded by- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef
- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 4,314 View
- 81 Download
- 1 Crossref

- Characteristics and Treatment Trends for Emphysematous Pyelonephritis in Korea: A 10-Year Multicenter Retrospective Study
- Seung-Kwon Choi, Koo Han Yoo, Jeong Woo Lee, Seung Il Jung, Eu Chang Hwang, Joongwon Choi, Woong Bin Kim, Jung Sik Huh, Jin Bong Choi, Yeonjoo Kim, Jae Min Chung, Ju-Hyun Shin, Jae Hung Jung, Hong Chung, Sangrak Bae, Tae-Hyoung Kim
- Urogenit Tract Infect 2021;16(2):49-54. Published online August 31, 2021
- DOI: https://doi.org/10.14777/uti.2021.16.2.49
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose: This study examined the characteristics, current treatment trends, and outcomes of patients with emphysematous pyelonephritis (EPN) in Korea.
Materials andMethods: Two hundred and seventeen patients diagnosed with EPN were evaluated using abdominal computed tomography in 2011-2021 at 15 institutes in Korea. The patients’ demographic and clinical characteristics, treatment modalities, and treatment outcomes were analyzed. The total study period was divided arbitrarily into groups A (2011-2014), B (2015-2017), and C (2018-2021) to analyze the trends in the EPN treatment.
Results: The mean age of the patients was 65.1 years; there were more female patients (74.2%) than male patients. The overall mortality rate was 10.6%. Ninety-five (43.8%), 98 (45.2%), and 24 (11.0%) patients were treated with medical, minimally invasive, and surgical management, respectively; the corresponding mortality rates were 13.7%, 6.1%, and 16.7%. There was no significant change in the proportion of patients treated with medical management over time (group A=46.5%, group B=47.0%, and group C=38.8%). The proportion of patients treated with minimally invasive management gradually increased over time (group A=35.2%; group B=43.9%; group C=55.0%), while those who underwent surgical management decreased gradually over time (group A=18.3%, group B=9.1%, and group C=6.3%). No differences in mortality rates were observed between the groups.
Conclusions: EPN with medical and minimally invasive management had a relatively high treatment success rate, which increased gradually, while surgical management decreased gradually over time in Korea. The mortality rate was relatively lower than that reported in studies published before the 2010s.
- 2,598 View
- 8 Download

- Clinical Characteristics and Antimicrobial Susceptibility of Elderly Women with Acute Pyelonephritis
- Ji Kang Yun, Woong Bin Kim, Sang Wook Lee, Kwang Woo Lee, Jun Mo Kim, Young Ho Kim
- Urogenit Tract Infect 2020;15(3):71-78. Published online December 31, 2020
- DOI: https://doi.org/10.14777/uti.2020.15.3.71
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose: Acute pyelonephritis in older patients can lead to a poorer treatment response and prognosis. The objective of this study was to classify older female patients with acute pyelonephritis according to age and compare their clinical characteristics and antibiotic susceptibility.
Materials and Methods: In this retrospective study, 360 patients aged 65 years or older and hospitalized for acute pyelonephritis in a single tertiary medical facility from 2012 to 2016 were selected as research subjects. The patients were divided into three groups according to their age. Their clinical symptoms, blood tests and urinalysis, underlying diseases, causative organisms for urinary tract infections (UTIs), and antibiotic susceptibility were compared.
Results: One hundred and seventy-six patients aged 69.9±2.7 years, 142 patients aged 79.4±3.1 years, and 42 patients aged 87.3±3.1 years were assigned into the young-old, old-old, and oldest-old groups, respectively. The duration of hospitalization and fever due to acute pyelonephritis increased with age. On the other hand, the maximum body temperature was similar among the three groups. In blood tests, erythrocyte sedimentation rate and C-reactive protein increased with age. Among the underlying diseases, the incidence of diabetes and chronic renal disease was similar among the three groups, while cerebrovascular diseases, heart failure, and urinary stones were associated with aging. Older patients were more likely to have UTIs over the past year. Older groups showed a more significant decrease in sensitivity to carbapenems, amikacin, and ciprofloxacin.
Conclusions: Choosing appropriate antibiotics, considering the patientʼs age, is important when treating acute pyelonephritis.
- 4,586 View
- 26 Download

- Risk Factors of Febrile Urinary Tract Infection after Ureteral Reimplantation in Infant
- Seungsoo Lee, Jae Min Chung, Sang Don Lee
- Urogenit Tract Infect 2020;15(2):33-37. Published online August 31, 2020
- DOI: https://doi.org/10.14777/uti.2020.15.2.33
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose: Children with febrile urinary tract infection (fUTI) and vesicoureteral reflux (VUR) show significant morbidity. Few studies have examined the incidence of fUTI after ureteral reimplantation for congenital urinary tract anomalies, particularly in infants. Therefore, this study examined the incidence and risk factors of fUTI after ureteral reimplantation in infants.
Materials and Methods: Children under one year of age, who underwent ureteral reimplantation from July 2017 to December 2018, were reviewed retrospectively. The patients’ data were analyzed to evaluate the predictors of fUTI after ureteral reimplantation.
Results: Ureteral reimplantation was performed in 16 patients (25 ureters) at a mean of 8.9±2.8 months. The preoperative diagnosis was VUR 14 (87.5%), obstructive megaureter 1 (6.3%), duplicated ureter 1 (6.3%). Postoperative fUTI occurred in five patients (31.3%) during the follow-up period (average 9.6±5.9 months, range 3-18 months). UTI occurred at 40.8±16.6 (17-61) days after surgery. Fourteen ureters were implanted with a ureteral catheter for three days, and 11 ureters were implanted with a double J ureteral stent for six weeks. The children’s age, sex, surgical method, renal scar, reflux grade, laterality, persisting VUR, and presence of double J ureteral stent were not predictive factors for postoperative fUTI.
Conclusions: The incidence of fUTI after ureteral reimplantation in infants was 31.3%, and all fUTI occurred within two months after surgery. The risk factors associated with fUTI after ureteral reimplantation could not be predicted. -
Citations
Citations to this article as recorded by- Open vs. robot-assisted laparoscopic ureteral reimplantation in a contemporary pediatric cohort: a retrospective single-institution analysis
Suhaib Abdulfattah, Nicole J. Kye, Sanjay Aiyar, Emily Ai, Marina Quairoli, Meghan F. Davis, Karl Godlewski, Katherine Fischer, Christopher J. Long, Dana A. Weiss, Aseem R. Shukla, Arun K. Srinivasan, Sameer Mittal
Journal of Robotic Surgery.2026;[Epub] CrossRef - Analysis of risk factors for postoperative febrile urinary tract infection in children with primary vesicoureteral reflux
Wenting Pei, Yin Zhang, Qihang Sun, Long You, Min Chao, Ye Zhang
Journal of Pediatric Surgery Open.2026; 15: 100282. CrossRef - Etiological Agents of Urinary Tract Infection (UTI)
Rana Thamer Hadi Alkhafaji, M. Jayashankar
International Journal of Scientific Research in Science and Technology.2022; : 381. CrossRef
- Open vs. robot-assisted laparoscopic ureteral reimplantation in a contemporary pediatric cohort: a retrospective single-institution analysis
- 4,173 View
- 13 Download
- 3 Crossref


 KAUTII
KAUTII

 First
First Prev
Prev